Your new post is loading...
 Your new post is loading...
Administering the correct dosages to fight cancerous tumors can be a difficult balancing act. Too much of the radioactive drugs can cause harm to healthy tissue, but not enough will see the cancer cells survive and continue to spread. But a new technique developed at The Institute of Cancer Research in London may afford doctors an unprecedented level of accuracy in performing radiotherapy, using 3D-printed replicas of a patient’s organs and tumors to better determine how much radiation a tumor has received.
"A recent study from the University of Colorado suggests that the chemical resveratrol found in grape skins and in red wine can help block the cancer-causing effects of alcohol.
"Alcohol bombards your genes," says Robert Sclafani, PhD, investigator at the University of Colorado Cancer Center and professor of biochemistry and molecular genetics at the CU School of Medicine. "Your body has ways to repair this damage, but with enough alcohol eventually some damage isn’t fixed."
The body metabolizes alcohol by converting it to acetyl aldehyde, then uses aldehyde dehydrogenase (ALDH) to further convert it to acetic acid, which is excreted. Acetyl aldehyde, a partially processed state of alcohol, is a carcinogen that produces DNA "cross links" that can cause cell death.
If enough alcohol is consumed..."
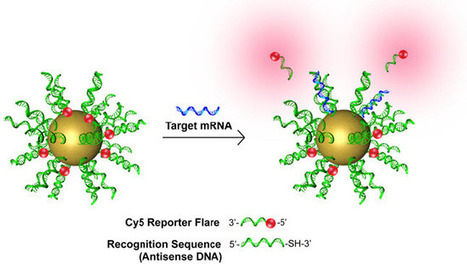
NanoFlares light up (red clouds) individual cells if a cancer (in this study, breast cancer) biomarker (messenger RNA, blue) is detected by recognition DNA
Engineers at Johns Hopkins Institute for NanoBioTechnology (INBT) have invented a lab device to give cancer researchers an unprecedented microscopic look at metastasis (spread of tumor cells, causing more than 90 percent of cancer-related deaths), with the goal of eventually stopping the spread, described in their paper in the journal Cancer Report.
Scientists at Dana-Farber Cancer Institute, the Massachusetts Institute of Technology, and other institutions have discovered a sign of the early development of pancreatic cancer – an upsurge in certain amino acids that occurs before the disease is diagnosed and symptoms appear. The research is being published online today by the journal Nature Medicine.
Although the increase isn't large enough to be the basis of a new test for early detection of the disease, the findings will help researchers better understand how pancreatic cancer affects the rest of the body, particularly how it can trigger the sometimes deadly muscle-wasting disease known as cachexia.
A polyphenol-rich supplement containing broccoli, green tea, tumeric, and pomegranete - a combination known as pomi-t - could have significant clinical benefits for men with prostate cancer, according to new data.
The proportion of U.S. men with early, slow-growing prostate cancer who received robotic surgery and other expensive treatments increased between 2004 and 2009, according to a new study. Researchers found that use of those therapies also rose among men who were unlikely to die from prostate cancer because they were sick with other chronic diseases when their cancer was diagnosed.
Led by researchers at Harvard School of Public Health (HSPH) and the Institute for Bioengineering of Catalonia (IBEC), investigators found that epithelial cells — the type that form a barrier between the inside and the outside of the body, such as skin cells — move in a group, propelled by forces both from within and from nearby cells — to fill any unfilled spaces they encounter. The discovery about how cells move inside the body may provide scientists with crucial information about disease mechanisms such as the spread of cancer or the constriction of airways caused by asthma.
A drug approved in Europe to treat osteoporosis has now been shown to stop the growth of breast cancer cells, even in cancers that have become resistant to current targeted therapies, according to a Duke Cancer Institute study. The findings, presented June 15, 2013, at the annual Endocrine Society meeting in San Francisco, indicate that the drug bazedoxifene packs a powerful one-two punch that not only prevents estrogen from fueling breast cancer cell growth, but also flags the estrogen receptor for destruction.
The early success of a new class of cancer drugs, revealed in test results released here over the last several days, has raised hope among the world’s top cancer specialists that they may be on the verge of an important milestone in the fight against the disease.
Diagnosed with advanced lung cancer over a year ago, Gabe Tartaglia was loath to undergo the kind of harsh chemotherapy that had devastated his sister before her death three years earlier from pancreatic cancer. He decided to enter a clinical trial for a new drug designed to trigger the immune system to fight cancer. The results were better than anyone expected.
A four-hour bath could release powerful anti-cancer proteins locked inside the hull of normal soybeans. (A Natural Cancer Drug From Soggy Soybeans?
|
Scientists have had some success activating the body's immune system to take the fight to cancer and other diseases, a process known as immunotherapy. Now, a new method developed by researchers at the Wyss Institute for Biologically Inspired Engineering at Harvard University could advance this form of treatment even further. The technique involves the injection of biomaterials that assemble into 3D scaffolds inside the body to accommodate huge amounts of immune cells, a process that could trigger an attack on deadly infections ranging from HIV to cancer to Ebola.
Cancer types such as melanoma, prostate cancer and certain types of leukemia weaken the body by over-activating the natural immune system. Researchers from the University of Copenhagen have now demonstrated that selenium -- naturally found in, e.g., garlic and broccoli -- slows down the immune over-response. In the long term, this may improve cancer treatment. The findings have been published in the Journal of Biological Chemistry.
In the spread of prostate cancer, the SRPK1 molecule is critical. It enables a tumor to generate new blood vessels and begin to grow. Research conducted at ...
In cancer treatments such as chemotherapy, hundreds of thousands of cancerous cells are killed off. But if even one of these cells has a unique mutation, it can survive the treatment and start to multiply, giving rise to a set of more drug-resistant cells. Researchers at the Salk Institute in California have now gained new insights into what exactly is causing these variations in the cells, suggesting there may in fact be a way of switching off the mechanism and improving treatment effectiveness.
Lead by staff scientist Fernando Lopez-Diaz, the Salk researchers set about identifying the diversification switch, that is, what mechanism was causing the cancers cells to multiply and take on slightly different forms. If this process could be prevented from happening, it may well curtail the cells' ability to develop the resistance to cancer-fighting drugs.
"Cancer isn’t one cell but it’s an ecosystem, a community of cells," says Beverly Emerson, professor at Salk's Regulatory Biology Laboratory. "This study begins the groundwork for potentially finding a way to understand and dial back cell diversity and adaptability during chemotherapy to decrease drug resistance."
A team of international researchers has developed a molecule capable of triggering cancer cell death by carrying chloride into cancer cell membranes. The molecule flushes the cells with salt and causes them to self-destruct, potentially paving the way for new types of anti-cancer drugs.The international effort involves researchers from the UK, Texas and South Korea who have collaborated to develop a synthetic ion transporter with a chloride payload. Once it reaches the cancer cells, the chloride interacts with the sodium in the cell membranes and leads to its demise.
Researchers at the Fraunhofer Institute for Interfacial Engineering and Biotechnology in Germany have created a miniature artificial lung that has the potential to significantly improve the process of developing treatments for lung cancer. In addition to the possibility of replacing animal trials currently used to test new medications, the "3D-lung" could be used to expand our understanding of how lung cancer spreads to the rest of the body.
With a volume of just half a cubic centimeter, the mini-lung has is made up of human lung cancer cells growing on tissue and is attached to a bioreactor that makes it "breathe" by pumping a nutrient medium through its blood vessels. The model is therefore able to react to medication the same as real human patients.
People who report eating the most red and processed meat before being diagnosed with colon cancer are more likely to die during the next eight years, according to a new study. "It's another important reason to follow the guidelines to limit the intake of red and processed meat," said Marjorie McCullough, the study's lead author from the American Cancer Society in Atlanta.
"Results showed that curcumin induces growth arrest and apoptosis in pancreatic cancer cell lines. Its effect was more obvious on the highly COX-2 expressing cell line..."
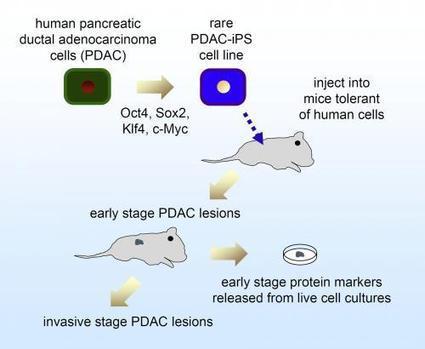
University of Pennsylvania scientists have used stem-cell technology to create a research cell line from a patient with advanced pancreatic ductal adenocarcinoma(PDAC). This first-of-its-kind human-cell model of pancreatic cancer progression was published this week in Cell Reports from the lab of Ken Zaret, PhD, professor of Cell and Developmental Biology. "It is the first example using induced pluripotent stem [iPS] cells to model cancer progression directly from a solid tumor, and the first human cell line that can model pancreatic cancer progression from early to invasive stages," says Zaret, also the associate director of the Penn Institute for Regenerative Medicine.
After being diagnosed with prostate cancer, men who eat a diet high in vegetable fats, such as those in nuts and olive oil, may be less likely to have their disease spread, a new study suggests.
Scientists at The University of Nottingham have found that a genetic rogue element produced by sequences until recently considered “junk DNA” could promote cancer progression. The researchers, led by Dr Cristina Tufarelli, in the School of Graduate Entry Medicine and Health Sciences, discovered that the presence of this faulty genetic element — known as chimeric transcript LCT13 — is associated with the switching off of a known tumor suppressor gene (known as TFPI-2) whose expression is required to prevent cancer invasion and metastasis. Their findings suggest that LCT13 may be involved in switching off TFPI-2.
Britain launched a research program on Monday that should eventually allow all cancer patients to have access to the kind of genetic analysis that led Hollywood star Angelina Jolie to decide to undergo a double mastectomy.
The project, involving the Institute of Cancer Research (ICR) in London, the U.S. gene sequencing firm Illumina, geneticists and cancer doctors, aims to find a way to allow more cancer genes be tested in more people.
|
 Your new post is loading...
Your new post is loading...
 Your new post is loading...
Your new post is loading...