Your new post is loading...
 Your new post is loading...
Scientists at the Georgia Institute of Technology have produced a new kind of paper that repels a range of liquids, including water and oil. The new paper shows significant promise as an affordable and recyclable packaging material, but it's the paper’s potential as an inexpensive biomedical diagnostic tool that has really got the researchers excited. By applying a chemical coating and creating new surface patterns at the nanometer and micron-scale, the researchers are able to reproduce the same repellent effect in the paper that is observed in the leaves of the lotus plant. This changes the paper from an absorbent material to one which repels all fluids.
Two children with an aggressive form of childhood leukemia had a complete remission of their disease—showing no evidence of cancer cells in their bodies—after treatment with a novel cell therapy that reprogrammed their immune cells to rapidly multiply and destroy leukemia cells. A research team from The Children’s Hospital of Philadelphia and the University of Pennsylvania published the case report of two pediatric patients Online First today in The New England Journal of Medicine. It will appear in the April 18 print issue. The current study builds on Grupp’s ongoing collaboration with Penn Medicine scientists who originally developed the modified T cells as a treatment for B-cell leukemias. The Penn team reported on early successful results of a trial using this cell therapy in three adult chronic lymphocytic leukemia (CLL) patients in August of 2011. Two of those patients remain in remission more than 2½ years following their treatment, and as the Penn researchers reported in December 2012 at the annual meeting of the American Society of Hematology, seven out of ten adult patients treated at that point responded to the therapy. The team is led by the current study’s senior author, Carl H. June, M.D., the Richard W. Vague Professor in Immunotherapy in the department of Pathology and Laboratory Medicine and the Perelman School of Medicine at the University of Pennsylvania and director of Translational Research in Penn’s Abramson Cancer Center. “We’re hopeful that our efforts to treat patients with these personalized cellular therapies will reduce or even replace the need for bone marrow transplants, which carry a high mortality risk and require long hospitalizations,” June said. “In the long run, if the treatment is effective in these late-stage patients, we would like to explore using it up front, and perhaps arrive at a point where leukemia can be treated without chemotherapy.” The research team colleagues adapted the original CLL treatment to combat another B-cell leukemia: ALL, which is the most common childhood cancer. After decades of research, oncologists can currently cure 85 percent of children with ALL. Both children in the current study had a high-risk type of ALL that stubbornly resists conventional treatments. The new study used a relatively new approach in cancer treatment: immunotherapy, which manipulates the immune system to increase its cancer-fighting capabilities. Here the researchers engineered T cells to selectively kill another type of immune cell called B cells, which had become cancerous. The researchers removed some of each patient’s own T cells and modified them in the laboratory to create a type of CAR (chimeric antigen receptor) cell called a CTL019 cell. These cells are designed to attack a protein called CD19 that occurs only on the surface of certain B cells. By creating an antibody that recognizes CD19 and then connecting that antibody to T cells, the researchers created in CTL019 cells a sort of guided missile that locks in on and kills B cells, thereby attacking B-cell leukemia. After being returned to the patient’s body, the CTL019 cells multiply a thousand times over and circulate throughout the body. Importantly, they persist for months afterward, guarding against a recurrence of this specific type of leukemia. While the CTL019 cells eliminate leukemia, they also can generate an overactive immune response, called a cytokine release syndrome, involving dangerously high fever, low blood pressure, and other side effects. This complication was especially severe in Emily, and her hospital team needed to provide her with treatments that rapidly relieved the treatment-related symptoms by blunting the immune overresponse, while still preserving the modified T cells’ anti-leukemia activity. “The comprehensive testing plan that we have put in place to study patients’ blood and bone marrow while they’re undergoing this therapy is allowing us to be able to follow how the T cells are behaving in patients in real time, and guides us to be able to design more detailed and specific experiments to answer critical questions that come up from our studies,” Kalos said. The CTL019 therapy eliminates all B cells that carry the CD19 cell receptor: healthy cells as well as those with leukemia. Patients can live without B cells, although they require regular replacement infusions of immunoglobulin, which can be given at home, to perform the immune function normally provided by B cells. The research team continues to refine their approach using this new technology and explore reasons why some patients may not respond to the therapy or may experience a recurrence of their disease. Grupp said the appearance of the CD19-negative leukemia cells in the second child may have resulted from her prior treatments. Unlike Emily, the second patient had received an umbilical cord cell transplant from a matched donor, so her engineered T cells were derived from her donor (transplanted) cells, with no additional side effects. Oncologists had previously treated her with blinatumomab, a monoclonal antibody, in hopes of fighting the cancer. The prior treatments may have selectively favored a population of CD19-negative T cells. “The emergence of tumor cells that no longer contain the target protein suggests that in particular patients with high-risk ALL, we may need to broaden the treatment to include additional T cells that may go after additional targets,” added Grupp. “However, the initial results with this immune-based approach are encouraging, and may later even be developed into treatments for other types of cancer.”
Via Dr. Stefan Gruenwald
Researchers at the University of Leeds are using the feet of tree frogs as a model for a tiny robot designed to crawl inside patients’ bodies during keyhole surgery.
It is designed to move across the internal abdominal wall of a patient, allowing surgeons to see what they are doing on a real-time video feed
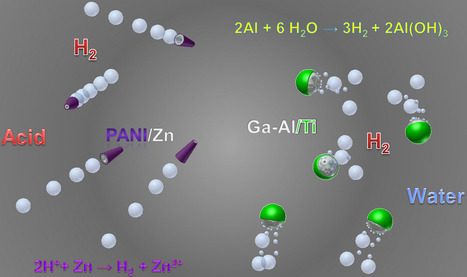
An advance in micromotor technology is opening the door to broad new medical and industrial uses for these tiny devices, scientists said the national American Chemical Society meeting this week. Akin to the invention of cars that fuel themselves from the pavement or air, rather than gasoline or batteries, Joseph Wang, D.Sc., who leads research on the motors, said that efforts to build minute, self-powered robot devices have evoked memories of the 1966 science fiction film Fantastic Voyage. It featured a miniaturized submarine, which doctors injected into a patient. It then navigated through blood vessels to remove a blood clot in the brain.
The most extensive bilateral arm transplant to date has been successfully achieved thanks to an interdisciplinary team of doctors and nurses at John Hopkins Hospital. The operation, which was performed on December 18, lasted 13 hours and involved 16 physicians from orthopedics, vascular medicine, plastic surgery, and other disciplines from five hospitals.
What if you could improve your memory, become smarter and stronger, and live in an ageless disease-free body – just by taking a pill? Though this may sound like the stuff of science fiction, experts are developing a better understanding of our genetic mysteries, including the powerful influence that DNA wields on our lives. It's becoming clear that cancer, heart disease, diabetes, obesity; most mental disorders, and many other ailments, could all be the result of a clash between genes we inherited from our past, and today's modern environment.
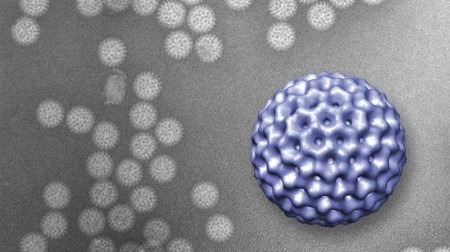
Scientists have developed a new technology that allows them to view live viruses in their natural habitat, as opposed to isolated frozen specimens.
When kidney stones can’t be dissolved using medication, the next step is usually a procedure known as shock wave lithotripsy. This involves focusing a series of high-intensity acoustic pulses onto the stones, until they break apart to the point that they can be passed in urine or dissolved by drugs. Using current monitoring techniques, however, it can be difficult to tell when and if that point has been reached. A new device known as the Smart stethoscope lets clinicians know, by listening.
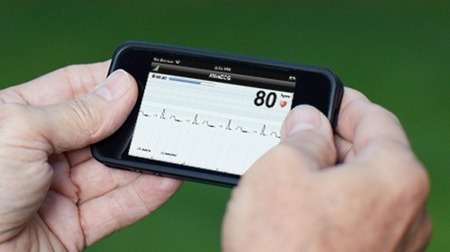
AliveCor’s smartphone Heart Monitor has received FDA approval and will go on sale to healthcare professionals in the United States in January 2013. The AliveCor Heart Monitor allows the recording, display, storing, transferring, and evaluation of single-channel electrocardiogram (ECG) rhythms using an iPhone 4 or 4S. The Class II medical device consists of a self-powered case that attaches to the back of an iPhone, which is running the associated heart monitor app. The phone and case communicate with one another wirelessly, though the phone doesn't need to be paired to the device.
NEW YORK (Reuters Health) - Among people with advanced cancer, poorer patients are less likely to be referred for clinical trials of experimental drugs, a new study from the UK suggests. Because those early trials will eventually help regulators decide if drugs should be approved for a wider population, it's important that test patients be representative of people the medications are designed to treat, researchers said. In addition, "There is an ethical issue of access to trials, because in general (for these patients), the standard therapeutic options have been exhausted," said James Spicer from King's College London and Guy's Hospital, who worked on the study.
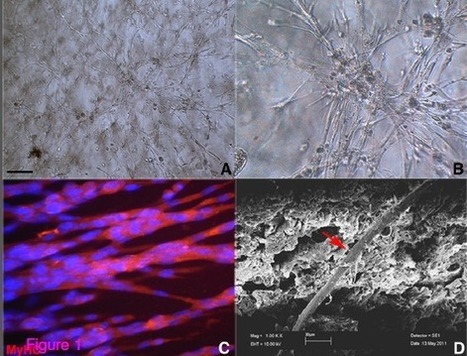
A new therapeutic technique to repair and rebuild muscle for sufferers of degenerative muscle disorders has been developed by an international team of researchers, according to a study published today in BioMed Central’s open access journal Skeletal Muscle. The therapy brings together two existing techniques for muscle repair — cell transplantation (mesoangioblast stem cells) and tissue engineering, delivering the stem cells via a hydrogel cell-carrier matrix.
The best medical innovations for next year include an almond-size device implanted in the mouth to relieve severe headaches and a handheld scanner resembling a blow dryer that detects skin cancer, the Cleveland Clinic said on Wednesday. The clinic's annual list of the best medical innovations for 2013 includes better mammography technology and new drugs to treat advanced prostate cancer.
A group of researchers at the University of Washington has found a way to isolate and identify medically interesting molecules using little more than scraps of office paper, a Ziplock bag and a cheap diluted solvent. If properly developed, the system – which requires minimal costs and know-how to build and operate – could be made to administer a wide range of medical tests nearly free of charge.
|
Researchers at Melbourne's St Vincent's Hospital is working on developing human organs by building body cells layer by layer using a 3D printer. The team has used the 3D printer to make body cells, including muscle cells, nervous systems cells and cartilage. Professor Mark Cook, director of neurosciences at St Vincent's Hospital, said 3D body part printing was like 'bubble jet printers'.
Patient says he felt back to normal eight days after procedure and has no enduring side effects (Clinical trial first for less invasive procedure to treat prostate cancer: Patient says he felt back...
The Internet of Things is coming, but chips need to be more efficient, powerful—and even smaller than they are now. In all categories, Freescale Semiconductor is making waves. And their most recent contribution, the Kinetis KL02, is one of the smallest microcontrollers in the world. Freescale’s press release makes no bones about it—this tiny chip was designed with the Internet of Things (IoT) in mind, “Space-constrained applications that previously couldn’t incorporate an MCU now can be upgraded to become smart applications, adding a new tier of devices to the IoT ecosystem.”
FutureMed 2013 has officially arrived. On Monday, Singularity University kicked off day one at their NASA Moffet Field campus, a stone’s throw from Hangar One and the NASA Ames Research Center. Seventy-five years ago this place housed giant airships—now the tech is smaller and exponentially more powerful. Which, of course, is what FutureMed is all about. To open the program, Director of FutureMed, Daniel Kraft, set the tone by delivering a whirlwind tour of exponential technologies and their impact on medicine and healthcare in the 21st century. Kraft said, “We’ve been flying blind.” But that’s changing fast. He went on to note how information technology is the basis of a vast and growing sensor network, connected real time at the speed of light. Smartphones can give EKG readouts or take blood sugar levels—and are increasingly able to analyze the data, provide initial diagnoses, and involve healthcare professionals as needed.
What if you could read my mind? What if I could beam what I’m seeing, hearing, and thinking, straight to you, and vice versa? What if an implant could store your memories, augment them, and make you smarter? Long the stuff of science fiction, technology that can directly tap into, augment, and connect human brains is becoming science fact. And that means big changes for all of us.
Seattle’s Presage Biosciences has developed a device which introduces small amounts of different chemotherapy drugs into a patient's tumor. The tumor is inspected after removal and the most effective of the drugs are used for post-surgical chemotherapy, resulting in more efficient, personalized cancer treatments. The new device is awaiting FDA approval, but is currently being used to facilitate development of new chemotherapy drugs.
One of the largest challenges faced by oncologists is finding an effective treatment for a particular patient that doesn’t cause the patient undue suffering.
Six medical innovations are poised to transform the way we fight disease, The Wall Street Journal reports. Surgeons at Boston Children’s Hospital have developed a way to help children born with half a heart to essentially grow a whole one — by marshaling the body’s natural capacity to heal and develop.Oxford Nanopore Technologies has unveiled the first of a generation of tiny DNA sequencing...
Mussels have an amazing ability to cling to rocks, even when buffeted by large waves and ocean debris on a daily basis. Now, scientists have created a bioadhesive gel inspired by those mussels, that could potentially be used to reinforce weakened blood vessels.
The gel, which was developed by a team at MIT, is capable of withstanding the flow velocity of the human bloodstream. It is said to be similar to an amino acid present in the mussel’s byssus – this is a fibrous adhesive material that's stiff enough to keep the mollusk in place, yet stretchy enough to flex without snapping.
TORONTO, ON — A medical sensor that attaches to the skin like a temporary tattoo could make it easier for doctors to detect metabolic problems in patients and for coaches to fine-tune athletes’ training routines. And the entire sensor comes in a thin, flexible package shaped like a smiley face... The new tattoo-based solid-contact ion-selective electrode (ISE) is made using standard screen printing techniques and commercially available transfer tattoo paper, the same kind of paper that usually carries tattoos of Spiderman or Disney princesses. In the case of the sensor, the “eyes” function as the working and reference electrodes, and the “ears” are contacts for a measurement device to connect to.
An implantable robotic arm controlled by thoughts is being developed by Chalmers University of Technology industrial doctoral student Max Ortiz Catalan in Sweden. Ever since the 1960s, amputees have been able to use prostheses controlled by electrical impulses in the muscles, their functionality is limited because they are difficult to control, according to Catalan.
Scientists from the University of Cambridge’s Veterinary School, working with colleagues from the UK Medical Research Council’s Regenerative Medicine Centre, have got disabled dogs walking again. More specifically, they’ve used the dogs’ own cells to repair their spinal cord injuries, and at least partially restored the functionality of their back legs. The researchers believe that the process shows promise for use on physically challenged humans.
Making a wheelchair that can deal with steps and other obstacles has puzzled engineers for decades, with everything from tank treads to spokes tried and found not quite practical. Now a team of engineers from the Chiba Institute of Technology, led by associate professor Shuro Nakajima, have applied a bit of lateral thinking. They have developed a robotic wheelchair that isn't sure what it is. Normally, it operates on wheels like a conventional wheelchair, but when it meets an obstacle, the wheels turn into legs.
|



 Your new post is loading...
Your new post is loading...