Adoptive transfer of genetically engineered chimeric antigen receptor (CAR) T cells is becoming a promising treatment option for hematological malignancies. However, T cell immunotherapies have mostly failed in individuals with solid tumors. Here, with a CRISPR–Cas9 pooled library, we performed an in vivo targeted loss-of-function screen and identified ST3 β-galactoside α-2,3-sialyltransferase 1 (ST3GAL1) as a negative regulator of the cancer-specific migration of CAR T cells. Analysis of glycosylated proteins revealed that CD18 is a major effector of ST3GAL1 in activated CD8+ T cells. ST3GAL1-mediated glycosylation induces the spontaneous nonspecific tissue sequestration of T cells by altering lymphocyte function-associated antigen-1 (LFA-1) endocytic recycling. Engineered CAR T cells with enhanced expression of βII-spectrin, a central LFA-1-associated cytoskeleton molecule, reversed ST3GAL1-mediated nonspecific T cell migration and reduced tumor growth in mice by improving tumor-specific homing of CAR T cells. These findings identify the ST3GAL1–βII-spectrin axis as a major cell-intrinsic program for cancer-targeting CAR T cell migration and as a promising strategy for effective T cell immunotherapy. CAR T cell success requires targeting tumors, but these cells can get trapped in other tissues, such as in the lungs, where they can cause pathology. Here, the authors use a loss-of-function CRISPR screen to identify regulators of CAR T cell tumor trafficking and engineer CAR T cells accordingly to overcome this limitation.
Research and publish the best content.
Get Started for FREE
Sign up with Facebook Sign up with X
I don't have a Facebook or a X account
Already have an account: Login
 Your new post is loading... Your new post is loading...
 Your new post is loading... Your new post is loading...
|
Pierre-Luc Jellimann 's curator insight,
October 26, 2022 9:01 AM
Découverte d'un vaccin thérapeutique utilisant les cellules cancéreuses (dénaturées) du patient afin d'entrainer le SI à reconnaitre et à éradiquer les cellules cancéreuses + mise en place d'une mémoire immunitaire sur plusieurs mois. Effet concluant chez des souris ayant un mélanome.
|




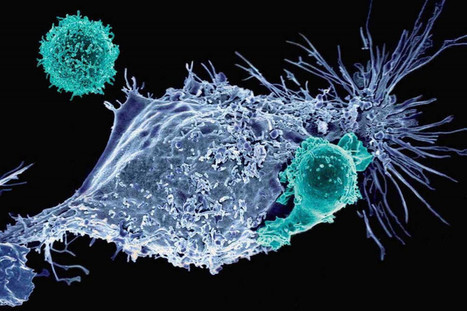

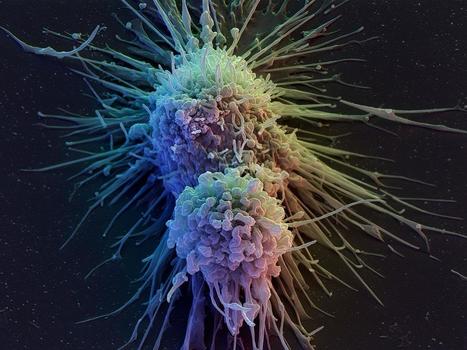
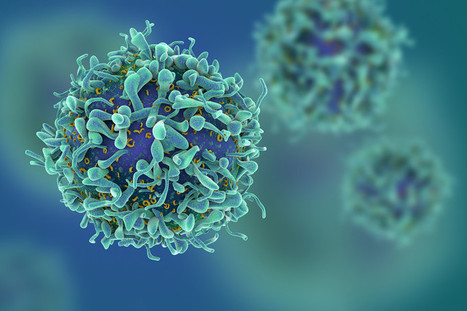


















Immunotherapy, particularly CAR T-Cell cancer therapy, extends the lives of many patients. But sometimes the therapy randomly migrates to places it shouldn't go, sneaking into the lungs or other non-cancerous tissue and causing toxic side effects. However, a team of researchers has discovered the molecule responsible for guiding T cells to tumors, setting the stage for scientists to improve the revolutionary treatment. Their discovery of the crucial migration control gene that expresses ST3GAL1 is the result of "unbiased genomic screening": researchers used a state-of-the-art CRISPR technique to edit thousands of genes expressed in T cells, then tested the migration control capabilities of these genes, one by one over a period of nearly four years, in mouse models. The next step is to find a drug that can manipulate the key T cell protein, ST3GAL1. If the study progresses as planned, such a drug could be added to the CAR T-cell regimen to ensure that the T cells reach their targets